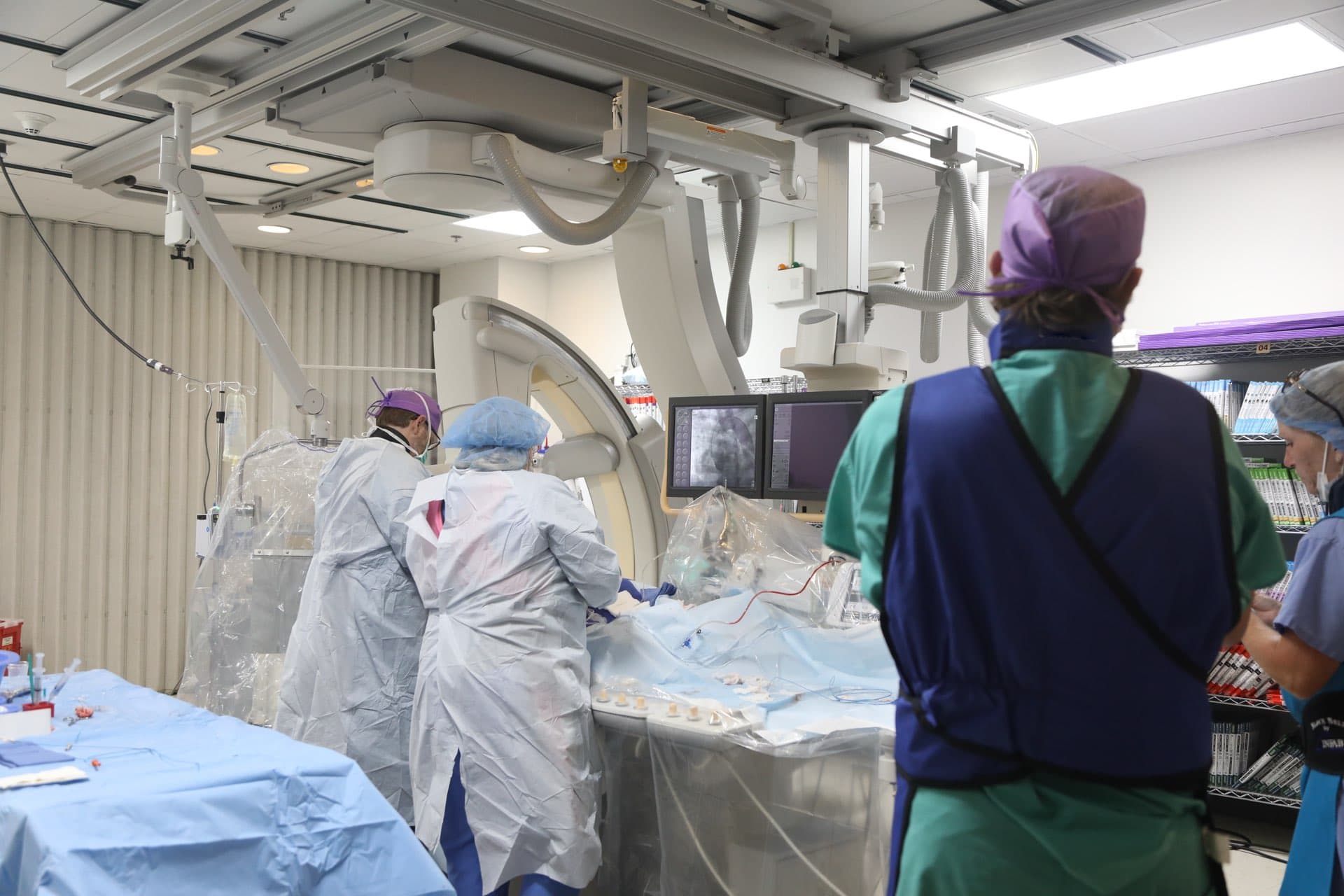
The short answer
What is ALARA+, in one paragraph?
ALARA+ stands for "As Low And as Light As Reasonably Achievable." It is the 2026 evolution of the decades-old ALARA radiation safety doctrine. Where the original framework only addressed ionizing radiation, ALARA+ also addresses the musculoskeletal injuries caused by the lead-equivalent garments worn to protect against that radiation. The "+" stands for Light. Nine medical societies endorse it. The summit paper that defines it was published in JSCAI on March 24, 2026.
Origin story
A brief history of ALARA
Modern radiation safety has a 70-year arc. Knowing where it came from is the only way to see what was missing.
- Step 011958
ALARA enters the regulatory vocabulary
The US Atomic Energy Commission articulates the principle that radiation exposure should be kept "as low as reasonably achievable" even when below legal limits.
- Step 021971
OSHA codifies the federal occupational standard
29 CFR 1910.1096 sets the rules that still govern radiation work in the US today. Interventional cardiology and interventional radiology do not yet exist as specialties.
- Step 031991
ICRP Publication 60
The International Commission on Radiological Protection adopts ALARA as a core protection principle and tightens occupational dose limits internationally.
- Step 042020
SCAI Multisociety Position Statement
Twelve societies publish "Occupational Health Hazards of the Catheterization Laboratory" calling for a paradigm shift in workforce protection. ORSIF is at the table.
- Step 052025
SCAI Think Tank in Washington
A multisociety summit reframes safety to include orthopedic injury caused by traditional lead protective gear. ORSIF participates and contributes economic data.
- Step 062026
ALARA+ formalized in print
"ALARA+: Summit on Radiation and Orthopedic Risks in Fluoroscopic Laboratories" publishes simultaneously in JSCAI, Heart Rhythm, JVIR, and JVS-Vascular Insights, endorsed by 9 societies.
The wins
Where ALARA worked
In any setting where the worker can step behind a wall, ALARA delivered. Three concrete wins in the healthcare context:
Patient dose, way down
Per-exam doses for routine CT and diagnostic radiography have fallen substantially over two decades. Modern fluoroscopy systems can cut patient dose by up to 65% without losing image quality.
Architecture as protection
Lead-lined walls, leaded glass, and ceiling-mounted shields are direct ALARA descendants. They protect the room, not just the person, and nobody has to wear them.
Dosimetry became a profession
Hospitals now employ medical physicists and Radiation Safety Officers (RSOs) whose entire job is monitoring dose, enforcing limits, and designing safer procedures. ALARA gave that role its mandate.
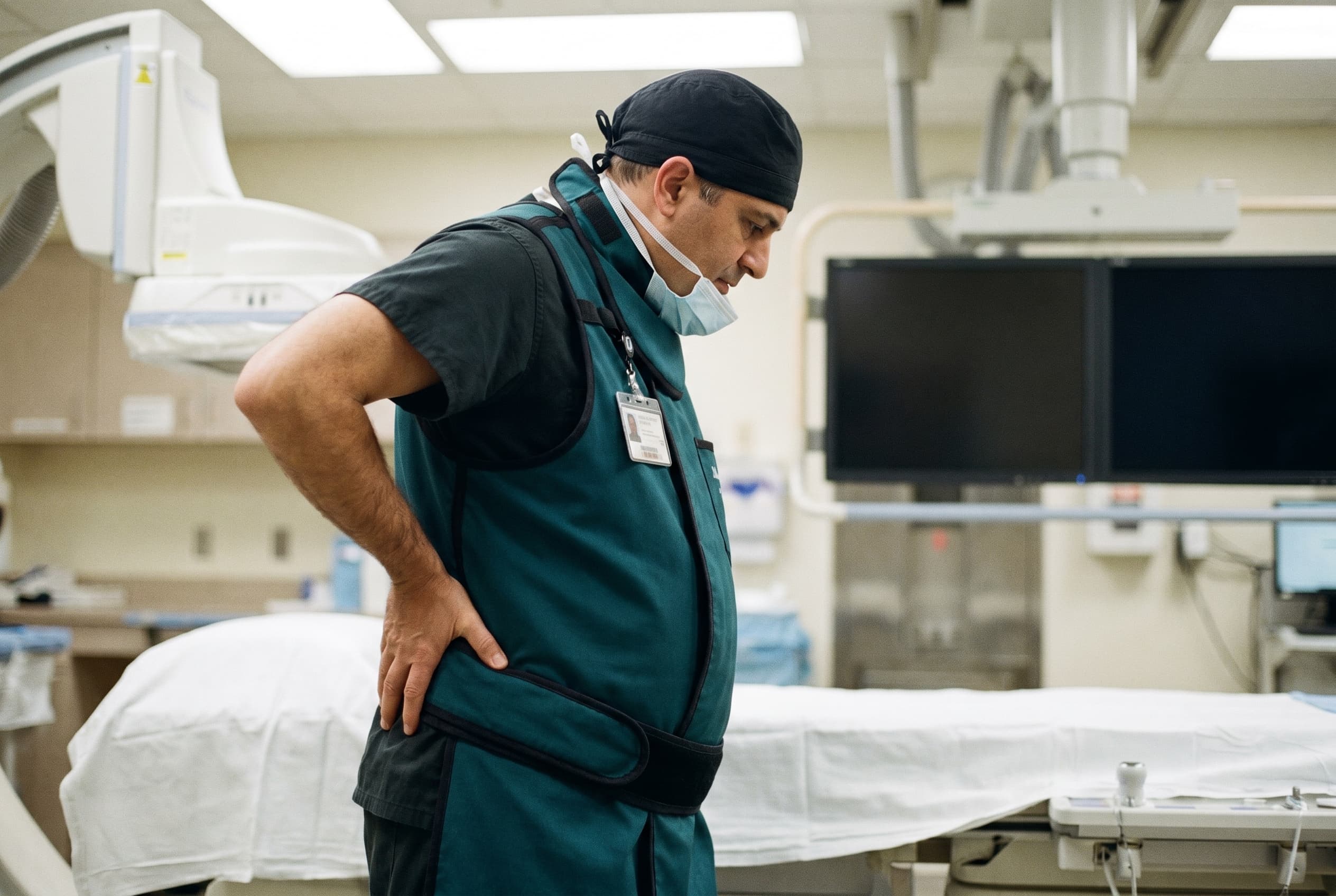
The break
Why ALARA fell apart in the cath lab
ALARA assumes a worker who can step away from the source. The interventional fluoroscopy lab is the opposite. The operator stands inches from the patient, who is the radiation source, for the entire procedure. Three of ALARA's foundational assumptions break here:
Distance is not available
Catheter-based procedures put the operator's hands and head inches from the patient's body, exactly where scatter radiation peaks. Two of ALARA's three classical levers, time and distance, are constrained by the procedure itself. Only shielding remains, and it has to be wearable.
The shielding became its own injury
Traditional Personal Protective Equipment (PPE) for fluoroscopy is a 15 to 20 pound lead-equivalent garment, worn for entire days of cases, often for whole careers. It causes documented neck, back, and shoulder injuries. The 2023 SCAI Occupational Health Hazards Survey found roughly two-thirds of interventional cardiologists report MSK pain related to the work or the gear. The mitigation became its own occupational disease.
The federal rule is older than the specialty
OSHA's ionizing radiation standard, 29 CFR 1910.1096, has not been substantively updated since 1971. Interventional cardiology and interventional radiology did not yet exist as recognized specialties. The rule still assumes a worker who is occasionally near a radiation source, not one who stands beside it 30 hours a week.
The reframe
ALARA+: same principle, different math
The 2025 SCAI Think Tank looked at the cath lab as it actually exists in 2026 and added one letter to the doctrine. The new framework reads: "As Low And as Light As Reasonably Achievable." Same underlying ethos. New scope.
| Axis | ALARA (1958) | ALARA+ (2026) |
|---|---|---|
| Acronym | ALARA | ALARA+ (the "+" stands for Light) |
| Stands for | As Low As Reasonably Achievable | As Low And as Light As Reasonably Achievable |
| Originated | 1958, US Atomic Energy Commission | 2026, SCAI 2025 Think Tank |
| Hazards covered | Ionizing radiation only | Ionizing radiation + musculoskeletal injury from PPE |
| Operator stance | Behind a wall, behind a barrier | Inches from the patient, all day, every day |
| Mitigation | Time, distance, shielding (lead PPE) | Engineered shielding + ergonomics + workforce policy |
| Workforce frame | Acceptable cost of doing the work | A retention and recruitment imperative |
| Endorsements | NRC, OSHA, ICRP, every regulator | 9 medical societies (SCAI, ACC, ACVP, ASE, HRS, SIR, SNIS, SVIN, SVS) |
"Traditional ALARA principles focused on incomplete methods of minimizing radiation exposure. They did not fully account for the orthopedic strain caused by wearing heavy lead protective equipment during long procedures. The new framework, ALARA+, calls for responsible protection strategies that are 'as low and as light as reasonably achievable' for the entire team."
ORSIF's role
ORSIF helped build it. Three receipts.
ORSIF (Occupational Radiation Safety in Interventional Fluoroscopy) is a 501(c)(3) advocacy organization built around the workers most exposed to the dual hazard. The summit paper documents three concrete connections, plus a bonus.
ORSIF is named in the Introduction
The summit paper's Introduction explicitly lists Occupational Radiation Safety in Interventional Fluoroscopy (ORSIF) among the professional societies represented at the SCAI 2025 Think Tank. We were in the room.
ORSIF's economic numbers anchor the case
The Financial Considerations section quotes ORSIF's estimates verbatim: $9M per fatal occupational cancer, $200K per nonfatal, $12K to $45K per MSK disorder. These are the headline numbers driving the financial case for change.
An ORSIF leader is in the author list
Robert E. Foster, MD appears in the co-author list of the peer-reviewed proceedings, published simultaneously across JSCAI, Heart Rhythm Journal, JVIR, and JVS-Vascular Insights.
ORSIF Advisory Board has the journal's Associate Editor
The paper's formal Declaration of Competing Interest discloses that David G. Rizik, MD serves on the ORSIF Advisory Board. Rizik is JSCAI's Associate Editor.
"However, ORSIF has estimated the cost associated with exposure to interventional fluoroscopy to be $9 million per case of fatal cancer, $200,000 per case of nonfatal cancer, and $12,000 to $45,000 per case of musculoskeletal disorder."
"David G. Rizik … serves on the executive physician council of Boston Scientific, on the medical advisory board of Abbott Vascular, and on the advisory board of Occupational Radiation Safety in Interventional Fluoroscopy (ORSIF)."
Who's behind it
Nine societies. One playbook.
The summit proceedings are formally endorsed by nine medical societies covering essentially every US clinician who works in a fluoroscopic environment.
ORSIF and the Society for Pediatric Radiology (SPR) also participated in the Think Tank as attendee societies.
The mandate
The four summit objectives
The summit organized the coalition's work under four objectives. Each is a lane the field can rally around.
Identify the hazards
Catalog every radiation and orthopedic risk to every person in the lab. Operators, imagers, anesthesiologists, technologists, nurses, fellows.
Connect safety to talent
Show how lab safety drives recruitment and retention, with attention to women in training and the underrepresentation of women in IC, EP, and neurointervention.
Untangle ERPD economics
Take on the cost barriers to Enhanced Radiation Protection Devices. List prices today are $150K to $200K, with reimbursement and regulatory gaps.
Issue a call to action
Publish specific, measurable steps the field can rally around. Real-time dosimetry. State-level advocacy. Manufacturer accountability.
The dual hazard, in numbers
Why a "+" was needed
Every figure below is drawn from the JSCAI summit paper or the ORSIF canonical statistics bank. The colored stripe at the top of each card flags the hazard category.
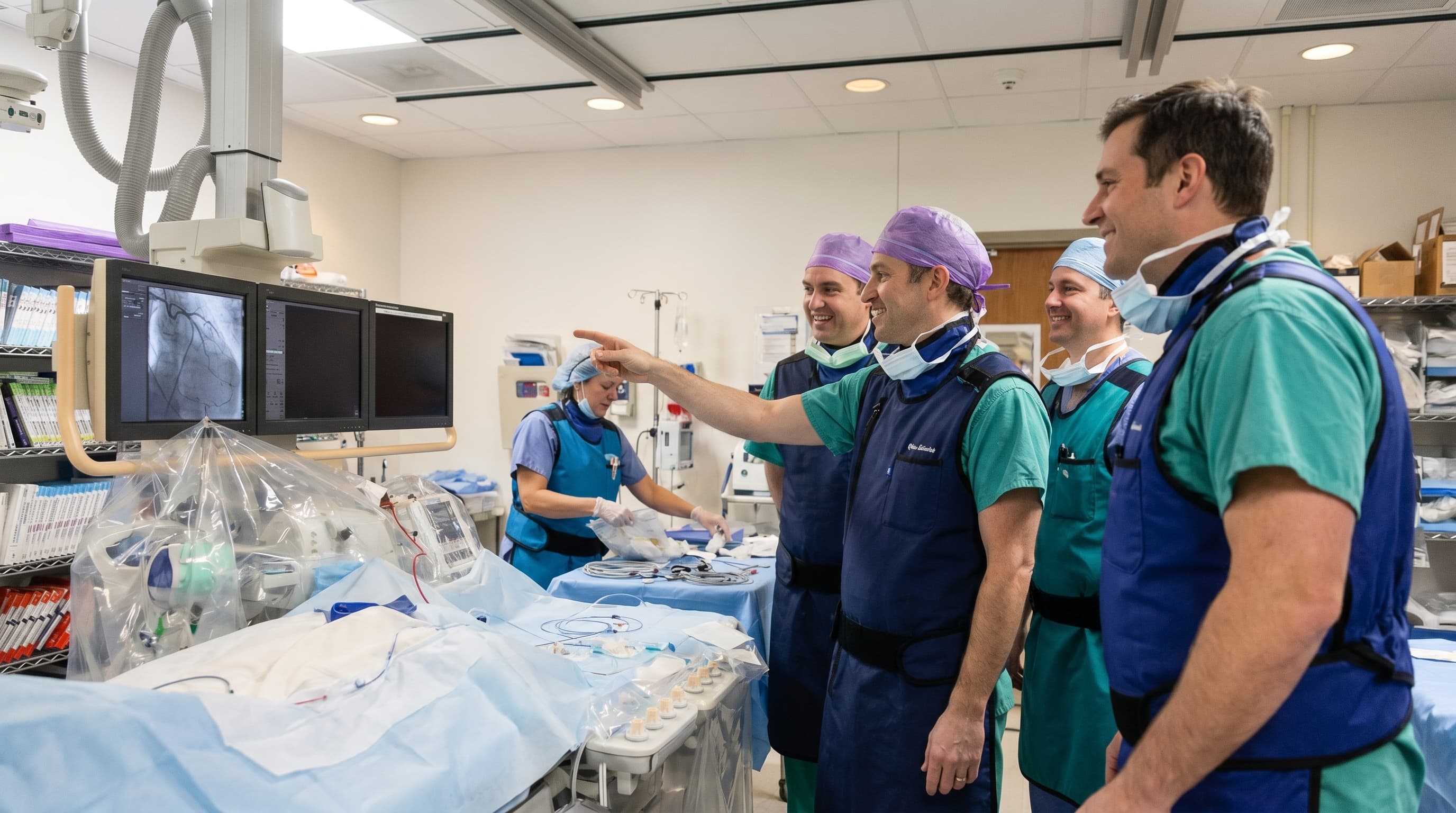
Operation Moral Imperative
"Effects of radiation exposure and the harmful physical sequelae of classic radiation protection mechanisms can no longer be the 'collateral damage' of the fluoroscopic laboratory."
The summit paper's Call to Action draws on the framing Dr. James B. Hermiller introduced in his 2024 SCAI Presidential Address. Advanced radiation protection technology, the paper argues, must become a mainstay of new catheterization laboratories and a retrofit priority for existing ones.
Salavitabar et al., JSCAI 2026, "Call to action" sectionWhere to go from here
Three things to do this week
ALARA+ gives the field a shared vocabulary. Turning that vocabulary into protection on the ground starts with three small actions.
Score your own risk
The 5-min ORSIF assessment turns the ALARA+ framework into a personal benchmark.
Take itRead the source library
621 peer-reviewed papers on occupational radiation and MSK safety. The same source pool the JSCAI paper cites.
BrowseFreeJoin ORSIF
Add your name to the only nonprofit focused on the dual hazard ALARA+ now formally recognizes.
Sign upFrequently asked
Common questions about ALARA+
Short, citable answers. Built for the questions search engines and AI assistants are most likely to ask.
What is ALARA+?+
ALARA+ stands for "As Low And as Light As Reasonably Achievable." It is the 2026 reframing of the longstanding ALARA radiation safety doctrine, expanded to also cover the musculoskeletal injuries caused by traditional lead-apron protective equipment. The "+" specifically marks the addition of "Light," meaning lighter physical burden on the operator.
How is ALARA+ different from ALARA?+
Traditional ALARA only addresses ionizing radiation exposure. ALARA+ addresses radiation AND the orthopedic burden of the lead-equivalent garments worn to protect against that radiation. The original framework assumed lead PPE was sufficient mitigation for the operator. ALARA+ recognizes that the PPE itself causes documented neck, back, and shoulder injuries in roughly two-thirds of interventional cardiologists.
Who endorses ALARA+?+
Nine medical societies formally endorse the ALARA+ summit proceedings: SCAI (Society for Cardiovascular Angiography & Interventions), ACC (American College of Cardiology), ACVP (Alliance of Cardiovascular Professionals), ASE (American Society of Echocardiography), HRS (Heart Rhythm Society), SIR (Society of Interventional Radiology), SNIS (Society of NeuroInterventional Surgery), SVIN (Society of Vascular and Interventional Neurology), and SVS (Society for Vascular Surgery).
When was ALARA+ formalized?+
ALARA+ was articulated at the SCAI 2025 Think Tank in Washington, D.C., and formally published on March 24, 2026 in the Journal of the Society for Cardiovascular Angiography & Interventions (JSCAI), with simultaneous co-publication in Heart Rhythm Journal, the Journal of Vascular and Interventional Radiology (JVIR), and the Journal of Vascular Surgery — Vascular Insights.
What is ORSIF's role in ALARA+?+
ORSIF (Occupational Radiation Safety in Interventional Fluoroscopy) participated in the SCAI 2025 Think Tank as one of the named professional societies. ORSIF's economic estimates ($9 million per fatal occupational cancer, $200,000 per nonfatal cancer, and $12,000 to $45,000 per musculoskeletal disorder) are cited verbatim in the summit paper's Financial Considerations section. David G. Rizik, MD, who serves on the ORSIF Advisory Board, is JSCAI's Associate Editor.
Is ALARA+ a regulation?+
No. ALARA+ is a multisociety consensus framework, not a federal or state regulation. The underlying federal occupational radiation rule, OSHA 29 CFR 1910.1096, has not been substantively updated since 1971. The coalition is calling for regulatory and accreditation modernization to align with the ALARA+ framework, but this is policy advocacy, not law.
What is an Enhanced Radiation Protection Device (ERPD)?+
An ERPD is a stationary, engineered shielding system that protects the operator from scatter radiation without requiring them to wear heavy lead garments. Current systems list at $150,000 to $200,000. ALARA+ calls for broader implementation of ERPDs as a way to address both halves of the dual hazard at once.
How can a healthcare worker apply ALARA+ today?+
Take the ORSIF 5-minute personalized risk assessment to benchmark your own radiation and musculoskeletal exposure profile. Read the JSCAI summit paper for the full multisociety consensus. Advocate within your institution for ERPD evaluation and for the kind of flexible work policies (especially for pregnant clinicians) that the summit paper specifically calls for.
Sources
Everything on this page is public, peer-reviewed, or society-published.
ALARA+: Summit on Radiation and Orthopedic Risks in Fluoroscopic Laboratories
Salavitabar A, Vora AN, Altschul D, et al. Co-published simultaneously in Heart Rhythm Journal, JVIR, and JVS — Vascular Insights. Lists ORSIF as a participating society, cites ORSIF's economic estimates verbatim in Financial Considerations (citation 46), and includes ORSIF Advisory Board member David G. Rizik on the editorial team.
Medical Societies Call for "ALARA+" Safety Standard
Official coalition announcement with quotes from Summit Chair Robert F. Riley, Co-Chair Arnold H. Seto, and SCAI President Srihari S. Naidu. Names all 9 endorsing societies and frames ALARA+ as a shift "from accepting risk to expecting better."
Radiation and Occupational Safety Resource Center
Organizes the summit proceedings, the 2020 Multisociety Position Statement, the 2026 ALARA+ toolkits (radiation safety, ERPD summary, economic argument, government advocacy), and on-demand education for the entire procedural team.
SCAI Multisociety Position Statement on Occupational Health Hazards of the Catheterization Laboratory
The 2020 multisociety statement that defined radiation, orthopedic, and reproductive risks and called for the paradigm shift in workforce protection that ALARA+ now formalizes. Cited throughout the 2026 summit paper.
ORSIF Economic Impacts of Radiation Exposures Associated with Interventional Fluoroscopy
The original ORSIF economic study cited as reference 46 in the JSCAI summit paper. Source of the $9M / $200K / $12K-$45K figures that anchor the coalition's financial argument.
Acronyms used on this page: As Low As Reasonably Achievable (ALARA); As Low And as Light As Reasonably Achievable (ALARA+); Personal Protective Equipment (PPE); Enhanced Radiation Protection Device (ERPD); Musculoskeletal (MSK); Interventional Cardiologist (IC); Electrophysiology (EP); Society for Cardiovascular Angiography & Interventions (SCAI); Journal of the Society for Cardiovascular Angiography & Interventions (JSCAI); Nuclear Regulatory Commission (NRC); International Commission on Radiological Protection (ICRP); Occupational Safety and Health Administration (OSHA); Radiation Safety Officer (RSO).
Last updated: April 28, 2026. ORSIF reviews this page quarterly to reflect new endorsements, regulatory developments, and updated coalition stats.